ADVERTISEMENTS:
Let us make an in-depth study of the nucleic acid metabolism. After reading this article you will learn about 1. Digestion and Absorption of Nucleic Acid and 2. Catabolism of Nucleosides.
Digestion and Absorption of Nucleic Acid:
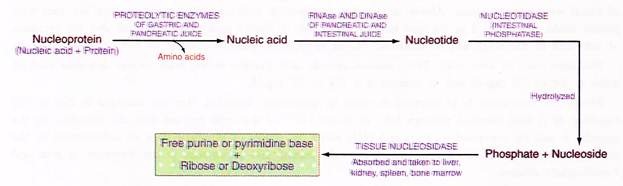
Nucleic acids are consumed in large quantities owing to their presence in all cells. These nucleic acids are not utilized by the body; instead they are digested, catabolized and excreted. They are taken in the form of nucleoproteins, which are conjugated proteins with amino acids constituting the protein part and nucleic acids constituting the prosthetic part.
The protein part of nucleoprotein is acted upon by proteolytic enzymes of gastric and intestinal juices. Nucleic acids are acted upon by nucleases (ribonuclease and deoxyribonuclease) of pancreatic and intestinal juices to produce mononucleotides. Nucleotides are hydrolysed to nucleosides by nucleotidases (intestinal phosphatase) Nucleosides are absorbed by intestinal mucosa to portal blood and transported to the liver and supplied through systemic circulation to other viscera. The enzyme nucleosides liberate the free purine and pyrimidine base and ribose or deoxyribose from the nucleosides.
Catabolism of Nucleosides:
1. Purine Nucleoside – Formation of Uric Acid:
End product of purine metabolism is uric acid (in primates including man and dog). In lower animals, birds and reptiles, uric acid is converted to allantoin by the action of enzyme uricase. Liver, spleen, kidney, intestinal mucosa contain enzymes capable of acting on the purine ring in the free or combined state.
Uric acid metabolism:
Uric acid exists as sodium ureate in plasma. Maximum amount of sodium ureate that can dissolve in the blood plasma is about 7 mg/100 ml. At this point there will be saturation of blood with sodium ureate. Above this it gets precipitated. Uric acid concentration does not vary with greater intake of uric acid in the diet because on intake of higher concentration in the diet the synthesis of uric acid in the body will be inhibited. Hence there is a balanced amount of uric acid in the body.
ADVERTISEMENTS:
Miscible pool of uric acid:
Total amount of uric acid present in the body in the dissolved state in males is 3.4 to 7.0 mg/dl and in females it is 2.4 to 5.7 mg/dl.
Modes of excretion:
It is excreted in urine by glomerular filtration. Amount excreted is 250 to 750 mgs/day. It is also excreted through bile, to about 1/5th of the total amount into the intestine. In the intestine it will be converted to CO2 and NH3 either by action of intestinal flora or autoxidation of the uric acid. Estimation of blood uric acid in ureotelic animals has importance in the diagnosis of gout and Von-Gierke’s disease.
Conditions varying the blood levels of uric acid:
Gout:
If the concentration of uric acid exceeds 7 mg/100 ml in the blood plasma, the uric acid gets precipitated as sodium ureate crystals that cannot be excreted hence gets deposited in the soft tissues. There is abnormal deposition in joints and tendons. This abnormal deposition of sodium ureate crystals in soft tissue is known as TOPHI. Because of this the tissue gets degraded or degenerated at the bone joints leading to degeneration of neighbouring tissues as well. Degeneration causes inflammation of the joint.
Gouty arthritis:
Generally the metacarpal phalangeal joints and metatarsal phalangeal joints are affected by this gout. Knee joint is also affected.
ADVERTISEMENTS:
There are two types of gout:
1. Primary Gout:
Enzyme ‘PRPP synthetase’ shows altered kinetics leading to overproduction of PRPP and hence overproduction of purines.
2. Secondary gout:
ADVERTISEMENTS:
This is due to—
(i) Excess catabolism of purine as in polycythemia.
(ii) Decreased excretion of uric acid as in renal failure.
Gout can be controlled by—
ADVERTISEMENTS:
1. Uricosuric drugs like salicylates, cinchopher, adrenal cortical hormones, which cause increased excretion of uric acid in urine by decreasing its re-absorption.
2. Allopurinol (Allantoin) a structural analogue to hypoxanthine which competitively inhibits xanthine oxidase and decreases the production of uric acid.
Von-Gierke’s disease:
In this disease there is an overproduction of uric acid. The HMP shunt pathway is overactive due to the deficiency of glucose-6-phosphatase thereby producing excessive amounts of ribose-5-phosphate. This leads to the overproduction of PRPP, hence the uric acid.
ADVERTISEMENTS:
Methods of estimation:
Phosphotungstic acid method, Fehling’s method and Auto analyzer.
Conditions varying the blood level of uric acids:
Whenever there is cell death, the nucleic acids are released and converted to purines and finally uric acid is formed.
The conditions where uric acid level increases in the blood are:
(a) Excessive tissue destruction and
ADVERTISEMENTS:
(b) Gout.
Excessive tissue destruction:
Is seen in—
1. Old age
2. Febrile diseases
3. Hypoxia
ADVERTISEMENTS:
4. Trauma
5. Kidney dysfunction or total renal failure
6. High non-vegetarian diets
2. Pyrimidine Nucleoside:
Pyrimidine nucleosides are catabolized in the liver. The products of breakdown of pyrimidine ring are ammonia and CO2 which are converted into urea for excretion.